|
8/31/2023 0 Comments Orif intertrochanteric fractureThis allows the many comorbidities with which patients often present to be optimized preoperatively, to reduce morbidity and mortality. Operative management of these fractures is considered urgent, not emergent. Unstable fracture patterns such as fractures with comminution of the posteromedial cortex, a thin lateral wall, displaced lesser trochanter fractures, subtrochanteric extension of the fracture and reverse obliquity fractures are also indications for intramedullary nailing. Fractures with involvement of the lateral femoral wall are considered an indication for intramedullary nailing and would not be treated with a sliding hip screw. The type of surgical treatment is based on the fracture pattern and its inherent stability, as the failure rate is highly correlated with the choice of implant and fracture pattern. The outcomes of this method of treatment are poor due to an increased risk of pneumonia, urinary tract infection, decubiti, and deep vein thrombosis. Nonoperative treatment is rarely indicated and should only be considered for non-ambulatory patients and patients with a high risk of perioperative mortality or those pursuing comfort care measures. Additionally, a physician-assisted AP traction view of the injured hip can be helpful in further characterizing fracture morphology and feasibility of closed reduction or need for open reduction techniques. MRI is indicated if there is an isolated greater trochanteric femur fracture and intertrochanteric extension is of concern. CT and MRI are typically not indicated but can be used if radiographs are negative, although the physical exam is consistent with a fracture. Full-length radiographs of the femur are useful to assess for deformities of the femur shaft which could affect the placement of an intramedullary nail and evaluation of prior implants in the distal femur. 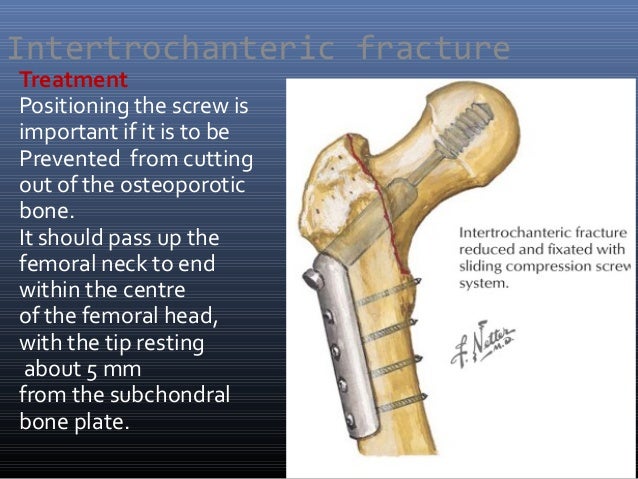
Although the diagnosis can be made without pelvic films, pelvic radiographs are useful to assist in preoperative planning for restoration of the proper neck-shaft angle. The recommended views include the anteroposterior (AP) pelvis, AP and cross-table lateral of the affected hip and full-length radiographs of the affected femur. Plain radiographs are the initial films chosen to evaluate for these fractures. In type II fractures, the A subclassification describes a 3 part fracture with a separate GREATER trochanter fragment while the B subclassification describes a 3 part fracture with a LESSER trochanter fragment. The A subclassification in type I fractures is used for non displaced fractures while B fractures are displaced. Type I is a 2 part fracture, Type II are 3 part fractures and Type III are 4 part fractures. 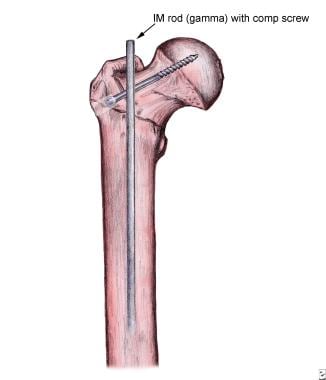
This Evans classification breaks down intertrochanteric femur fractures based on displacement, number of fragments and the type of fragment displaced. Examples of unstable fractures include: comminution of the posteromedial cortex, a thin lateral wall, displaced lesser trochanter fracture, subtrochanteric extension and reverse obliquity fractures. Stable fractures have an intact posteromedial cortex and will resist compressive loads once reduced. 
Determination of stability is important as it helps determine the type of fixation required for stability. These fractures are usually a result of a ground-level fall in the elderly population and are classified as either stable or unstable.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
